The intensive care unit – commonly called the ICU – is a floor or area of the hospital designed to care for children that require a lot of medical attention and support. The ICU is where your child will begin their recovery after cardiac surgery.
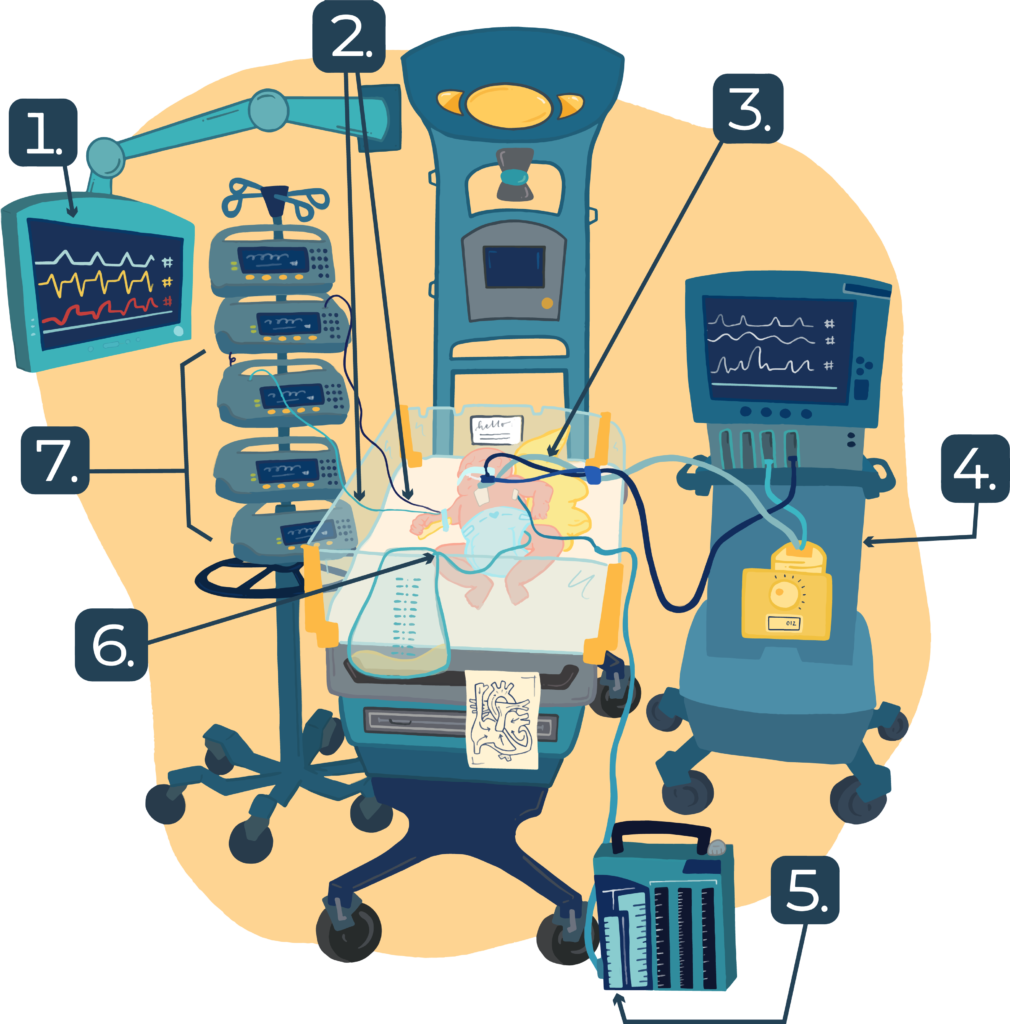
- Continuous monitor (Heart rate, oxygen saturation)
- Intravenous lines
- Endotracheal tube and Ventilator tubing
- Ventilator
- Chest tube and collection chamber
- Foley catheter
- Medication drips (via IV lines)
See additional equipment that you might find in the ICU
Nothing can prepare you to see your child for the first time after surgery or for the ups and downs that may happen in the ICU. Your child will have an incision in their chest and many tubes attached to give them medications and fluids, and to help them breathe and eat. Their heart rhythm and oxygen levels will be monitored every second of the day.
The ICU is a very intense environment that most people are not familiar with. Learning what to expect will help prepare you to support your child during the critical time they are recovering in the ICU.
Many people work together in the ICU to help your child through recovery. It may be difficult to get oriented when your child first arrives, but you will gradually become more familiar with the people and routines.
The care team knows that this can be a stressful and emotional time for your family. It’s okay to ask questions so that you understand what’s happening and feel comfortable with your child’s care. It’s important to talk with the care team about any concerns you have or changes that you notice in your child’s condition.
Basic Things to Know About the ICU
Good Hygiene Is a Priority
Preventing infection is a big focus in the ICU because the children are vulnerable while their bodies are trying to heal. To help keep the risk of infection low, you will be asked to wash or sanitize your hands every time you enter and leave the ICU. If you or a family member is sick, please stay home for the health of your child and the other patients.
It’s a Little Different at Every Hospital
At your hospital it may be called the ICU or PICU (Pediatric Intensive Care Unit), or there may be a separate CICU (Cardiac ICU) or CVICU (Cardiovascular Intensive Care Unit). In some hospitals there’s a cardiac ICU that only cares for children with heart problems, while other hospitals treat children with all conditions in one general pediatric ICU.
The Front Desk Can Always Help You
All ICUs have a front desk where someone greets you and can answer your general, non-medical questions. This includes rules like visiting hours, numbers of visitors, and bringing in outside food or personal items. If the front desk clerk cannot answer your question, they can direct you to a person who can.
It’s a Busy Place
An ICU can only run smoothly when a big team works together, because each person has a different focus or specialty. Medical professionals are constantly evaluating and providing care for all of the patients – sometimes this includes performing medical procedures. Patients are regularly arriving and leaving for surgeries and tests in other parts of the hospital.
What to Expect When Your Child Is in the ICU
Key Members of Your Child’s ICU Care Team
Learning how to communicate with your care team in the hospital is critical as you partner with these and other medical professionals to support your child’s recovery.
1. Nurses
A charge nurse is always on duty in the ICU to oversee the many types of nurses and the medical unit. A key member of the nursing team is the bedside nurse assigned to your child. They closely monitor your child, give medications, and communicate any issues with the rest of the ICU team. The bedside nurse also helps keep you generally informed about your child’s condition.
2. Physicians
The physician team cares for a group of patients. This team may include physicians, residents or fellows (physicians getting extra training in an area of medicine), and physician assistants. They are led by the attending physician, who is a physician with specialized training in ICU care or pediatric cardiology.
3. Surgeons
The surgical team may also visit your child in the ICU. This team may include surgeons, resident or fellow surgeons, physician assistants, and nurse practitioners. They may help manage your child’s surgical wounds, perform minor procedures at the bedside if needed, and discuss care with the medical team.
4. Other Medical Professionals
Many people work in the ICU. Respiratory therapists manage breathing equipment and provide respiratory treatments to help your child’s lungs recover after surgery. Your child may also have a dietician, social worker, physical therapists, pharmacist, and child life specialist, among other support.
PARENT TIPYou Are Essential to Your Child’s Recovery
The care team encourages parents to be at their child’s bedside. You are a source of familiarity and comfort for your child during this hard time. You know your child best and can help the team understand their needs and feelings.
Expect Ups and Downs in the ICU
There may be complications as your child recovers. This is common in the ICU, but it can be frustrating for you and your child. The ICU is designed to allow the team to identify changes quickly and respond as needed. Your ICU team is there to talk with you about any issues that arise – whether they are expected or unexpected, how they might change your hospital stay and child’s recovery, and how best to treat them.
FAQs
Rachel Kotheimer, Parent
Danielle Sganga, Physician
Theresa Tacy, Physician
See the full list of contributors to the CHD Care Compass
Last Update: November 3, 2021